Sponsored
From postpartum to menopause, it’s time to talk about female incontinence
Sponsored By

By IMAGE
30th Jun 2022
30th Jun 2022
Sponsored By

Did you know that incontinence affects one in every three women? We talk to consultant urologist James Forde about signs, symptoms and treatments.
When talking about female health, urinary incontinence is often left out of the conversation. And while it’s not the most glamorous subject to discuss, it is a very normal part of life, especially for women.
In fact, incontinence affects twice as many females as males. This is down to a number of reasons, often including menopause, childbirth and ageing.
But why do these important life stages frequently cause this issue? James Forde, consultant urologist at Blackrock Clinic, breaks it down for us in this FAQ guide.
What exactly is female incontinence?
“Urinary incontinence means the loss of bladder control and is an extremely common problem. The severity ranges from occasionally leaking urine when you cough or sneeze to having an urge to urinate that’s so sudden and strong you don’t get to a toilet in time.”
What are its common causes?
“The two most common types of urine leakage in women are stress urinary incontinence and urgency urinary incontinence. In some cases women may have mixed incontinence, which means they have both stress and urge incontinence.”
- Stress incontinence is usually caused by the weakening of or damage to the muscles used to prevent urination, such as the pelvic floor muscles and the urethral sphincter.
- Urge incontinence is usually the result of overactivity of the bladder (detrusor) muscles, which control the bladder.
“Certain things can increase the chances of urinary incontinence, including pregnancy and vaginal birth, obesity, family history of incontinence and increasing age.”

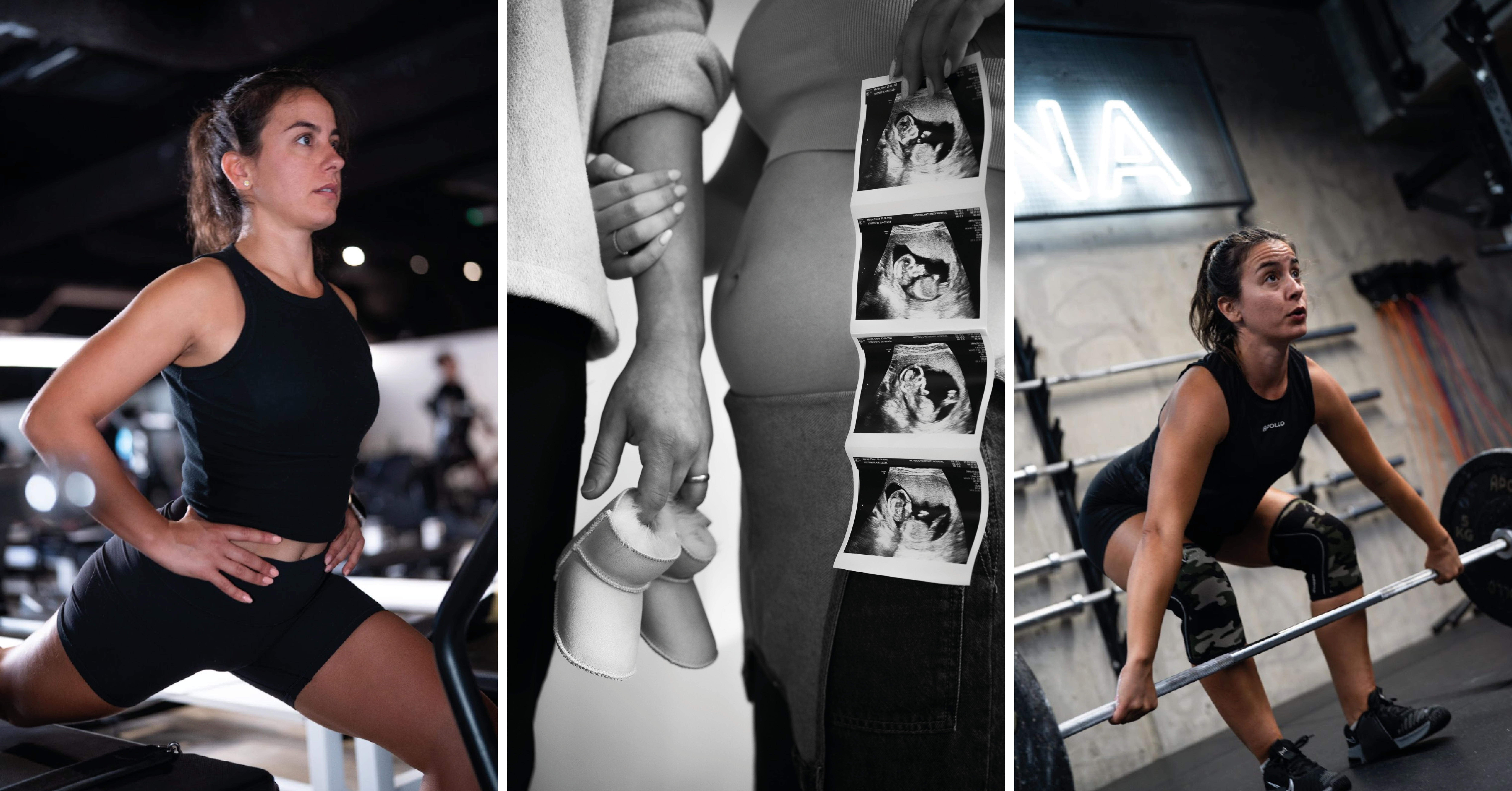
Postpartum
There are two main reasons why women often experience postpartum incontinence: hormonal changes and a weakened pelvic floor.
“During pregnancy, increased pressure from the weight of the foetus can lead to stress incontinence, while in childbirth, vaginal delivery can weaken muscles needed for bladder control and damage bladder nerves and supportive tissue,” explains Forde. “This leads to a pelvic floor weakness which may be associated with incontinence.”
Menopause
Once again, hormonal changes are at play when it comes to menopausal incontinence. “After menopause, women produce less oestrogen, a hormone that also helps keep the lining of the bladder and urethra healthy, and deterioration of these tissues can aggravate incontinence,” says Forde.
“Also, ageing of the bladder muscle can decrease the bladder’s capacity to store urine, and involuntary bladder contractions become more frequent as you get older.”
What treatment options are available?
There are plenty of treatments available, says Forde, but when it comes to choosing the best one for you, you have to consider the following: the type of incontinence you have, the severity of your symptoms and if it could be caused by an underlying medical condition. (If it is, you may need additional treatment).
“Non-surgical treatments are tried first and are usually managed by your GP along with a continence nurse advisor, physiotherapist or other allied health professionals. These include lifestyle changes, pelvic floor muscle training (such as Kegel exercises) and bladder training.”

- Lifestyle changes usually involve changing the type and amount of fluid taken. Reducing the amount of caffeinated drinks and excessive fluid intake are important first steps. Losing weight may also help.
- Pelvic floor exercises, where you strengthen your pelvic floor muscles by squeezing them, can be effective and you may be referred to a specialist physiotherapist to learn these exercises.
- Bladder training, where you learn ways to wait longer between needing to urinate and passing urine, can sometimes help with the daily management of this issue.
- Incontinence products like absorbent pads help benefit many women who suffer from incontinence. If you’re not sure where to start, Always Discreet are a great option – they’re light and comfortable with ‘leakguard’ and ‘odourlock’ technology as well as a unique triple layer core for superior protection.
“If these treatments fail to improve symptoms medication or surgery may be considered,” says Forde. “This conversation can be had with your GP who may consider referring you to a urologist or gynaecologist with a special interest in female incontinence.”
“Overall, female urinary incontinence is an extremely common condition affecting many on a daily basis and can often impact their quality of life,” says Forde. “There are many treatment options available and starting the conservation with your doctor can hopefully lead to significant improvements.”
The Always Discreet range has unique triple layer core technology that allows for superior comfort and discretion, as 30 per cent of women have identified the ‘bulkiness’ of incontinence products as a barrier to purchase. Shop the range online or in-store at TBC.