by Lauren Heskin
05th Feb 2024
05th Feb 2024
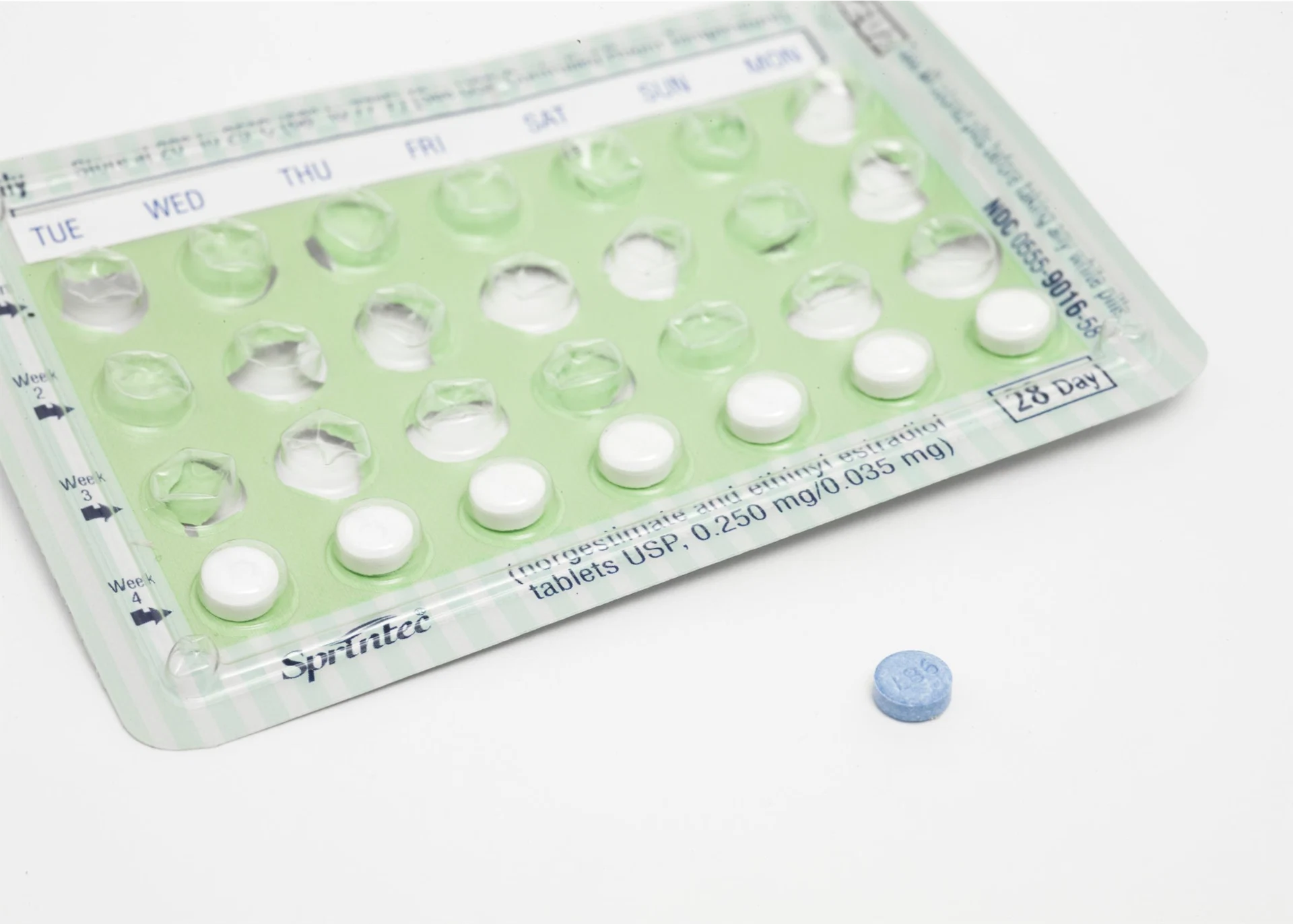
The pill
After 10 years of taking it religiously, I started to wonder exactly what it was that I was putting into my body every day.
I remember the first time I asked for the pill. The GP who attended to me – I avoided the family doctor out of teenage awkwardness – talked relentlessly about how women always complained about their boobs getting bigger when they were on the pill when really it was just water retention and it should subside after a few months. I hadn’t heard of this before and frankly, it wouldn’t have deterred my gangly 16-year-old...
You have reached a premium article.
For unlimited digital access to the stories worth paying for, subscribe now to IMAGE from just €4.99 a month
LoginSubscribe