premium
‘I was so terrified my kids would be taken away if I admitted how badly I was struggling’
by Amanda Cassidy
21st Oct 2020
21st Oct 2020
Research has found those experiencing perinatal depression (1 in 5 of us) don’t know where to seek help. Amanda Cassidy speaks to mums who share their experience “It took me two and a half years to come to the realisation that I was suffering from post-natal depression," admits Elaine Platt, an Amatsu therapist and mum to Wesley and Amelia. "And the thing that got me was the hushed tones that others would talk about it......

You have reached a premium article.
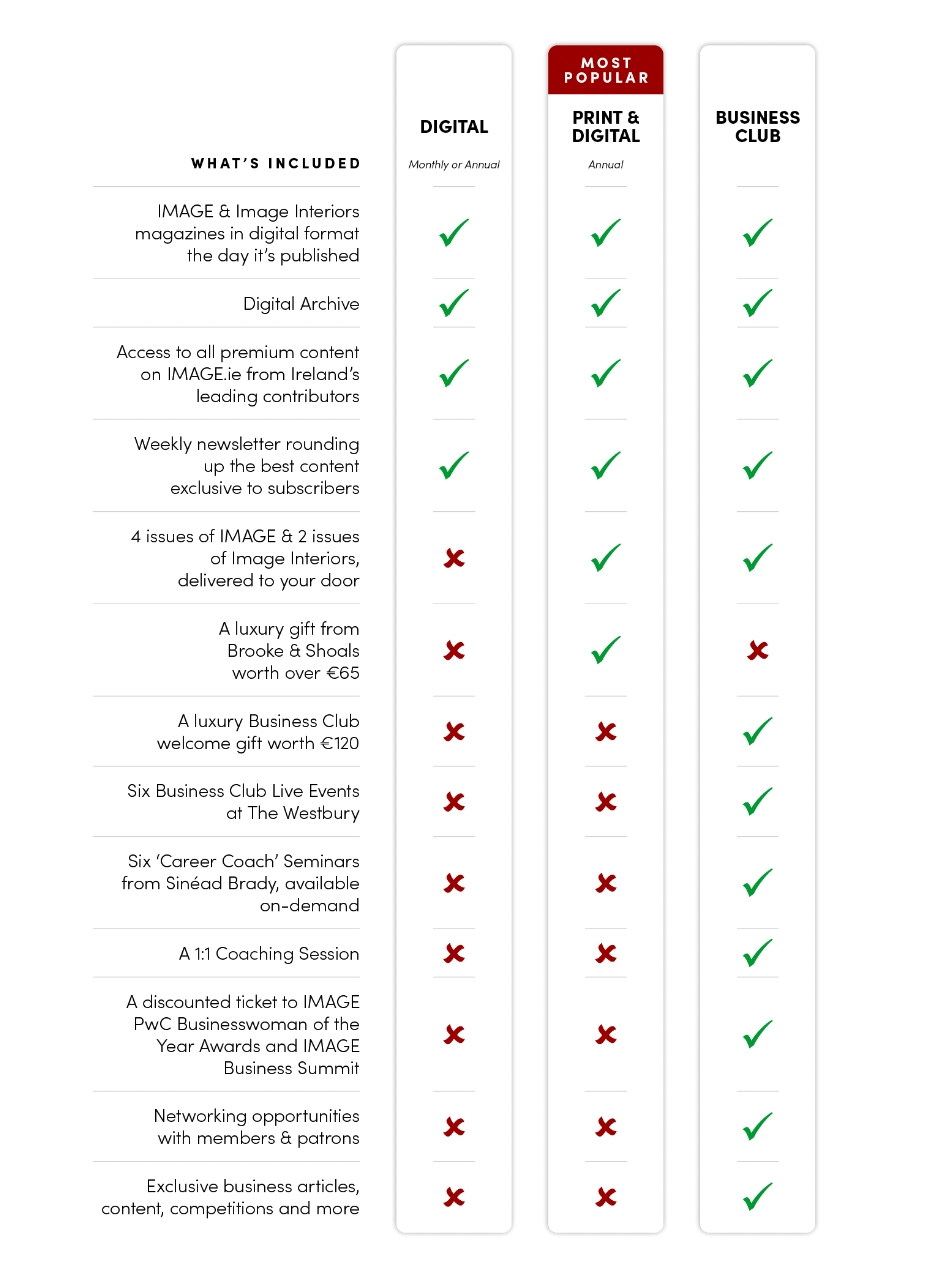
For unlimited digital access to the stories worth paying for, subscribe now to IMAGE from just €4.99 a month
LoginSubscribe