By IMAGE
28th Sep 2015
28th Sep 2015
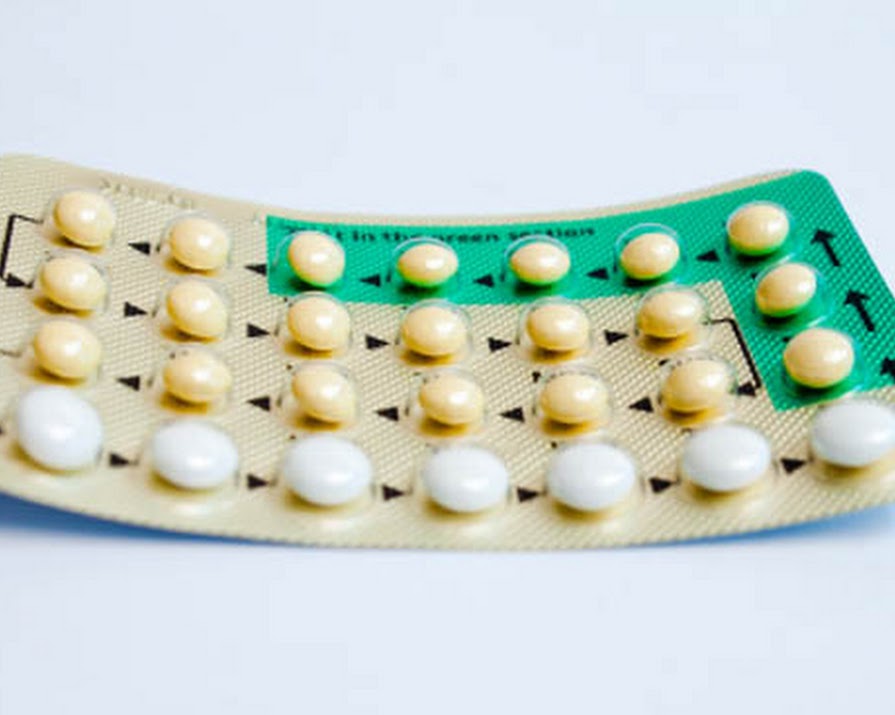
This weekend, when we weren’t busy celebrating Ireland’s win in the Rugby World Cup, we were schooling ourselves in the world of contraception. How much do we know? Are we as well-informed as we should be? Are we aware of our options and the risks associated with each form of contraceptive??To mark World Contraception Day, Bayer Healthcare ‘released a new ?Truth Report?, finding that Irish women in their twenties want more information about sex and contraception. Here we consult the wisdom of Dr. Sinead Beirne, GP to bring us up to speed on something that affects us all.
1. Looking at these statistics, Irish women are a lot less informed on all things contraception than we might have thought, is this surprising?
This doesn’t completely shock me. I find as a GP that women aged 20-29 often start on a type contraception (often the pill) and they just keep renewing it, not questioning whether there’s something better and more reliable option available. This is despite the fact that the pill may not suit their busy lifestyle, as it’s just another thing to have to think about everyday.
Perhaps we are all a little guilty of inertia; I know I am when it comes to certain things like car insurance. We’re afraid of change. The same happens with contraception. Once a woman has started with the pill, they often don’t change, even though there are far more reliable and cheaper options out there.
In comparison, I find my female patients in their 30’s are much more informed about other contraceptive options such as LARC (Long Acting Reversible Contraception). Maybe this is because they talk about it more openly with their friends. These days, Irish women are having their children in their 30’s. This group are usually very aware of LARC, and it’s a popular choice for family planning.
I think women are more open in their 30’s about sharing their experiences of contraception with their friends. At this slightly older stage contraception seems less of a taboo subject and just a practical fact of life.?I think it’s ironic in a sense that women in their 30’s are much more aware of LARC (the most reliable form of contraception) compared to women in their 20’s. Millennial women are even more fertile than women in their 30’s, they have more unsettled lives and are are at higher risk of unplanned pregnancies. So really it would make more sense if women aged 20-29 years were aware of the most reliable contraception like LARC.
2. Where are Irish women expected to become informed?
I think the best place for Irish women to become informed is in their GP surgery. As a female GP, contraception is my bread and butter. GP’s know their patients well and what life stage they are at. We know your medical history, which is really important because not all contraception is suitable for everyone.
You need to be careful when you’re looking up information online. There’s a lot of misinformation and inaccurate information out there. If you read something health related on the internet, don’t be afraid to ask your GP to double-check it.
There’s a great website that I’d recommend called www.mycontraception.ie. It’s really easy to follow, and it’s a great reference for all types of contraception.
41% of Irish women want to know more about sexual performance, sexual positions and reaching orgasm
3. There’s still a lingering embarrassment around the subject of sex, do you think that’s improving?
I think Ireland has come a long way in the past 50 years. If you think about it, the pill has only been available since the 1960’s. Until 1978, it was illegal to use the pill in Ireland, and you had to prove that it was for the purpose of family planning or for adequate medical reasons. Condoms were also banned until about 1985 and even then they weren’t widely available. So it’s a very different Ireland now. I think women probably feel more comfortable talking about sex and contraception with female doctors. As a GP I find my female patients are usually very comfortable talking about these things in the consultation room. After all, it is a fact of life and it’s great to see people taking responsibility for their sexual health.
58% of Irish women admit to sharing information on sex or contraception with others without knowing if it was accurate
4. Right now, what are the contraceptive options available to Irish women?
Wow, there’s so many. But it’s important to remember that not every option is suitable for every woman. That’s why it’s important to discuss your individual needs with your GP.?To summarise there are Long-Acting Reversible Contraceptives (LARCs) and Short-Acting Hormonal Contraceptives.?The LARCs are the most reliable because you don’t have to remember to take them daily, weekly or monthly. They can last anything from 3 months up to 10 years and include the Intrauterine System (IUS), the Intrauterine Device (IUD), the injection and the Sub-Dermal Implant.?The really great thing about LARC is that although LARC can potentially last for a long time, once you stop taking them your fertility returns to normal. This is with the exception of the injection in which fertility can take longer to return to normal.
The Short-Acting hormonal contraceptions include the combined pill (what we usually just refer to as ?the pill?), the progesterone-only pill, the contraceptive patch and the vaginal ring. The Short-Acting hormonal contraceptives are highly effective too. However you need to be really organised and meticulous about talking then correctively.
There are also barrier methods including male condoms, female condoms, diaphragms and spermicides. These have the benefit of not having any hormone for those who’d prefer to avoid hormones. The effectiveness of barriers depends entirely on the experience of the person using them.?I always encourage women in their 20s to use condoms regardless of what other contraception they’re using to help avoid sexually transmitted infections.
1 in 6 Irish women in their 20’s feel ill-informed about the facts on sex and contraception
5. How are Irish women to know what will work best for them?
As I mentioned earlier, your GP is a great person to discuss all of the contraceptive options with. They will be able to go through the pros and cons of each. They will also be able to give you reliable, practical advice.?If you’d prefer to do your own research, there is a brilliant website called www.mycontraception.ie that goes through everything. Remember, knowledge is power!
6. Can you tell us a little more about the long-acting reversible contraception?
Long-acting reversible contraception (or LARC) is a method of contraception that is highly effective in protecting a women from getting pregnant for more than one year. LARC includes the Intrauterine system (IUS), Intrauterine Device (IUD), the injection and the sub-dermal Implant.?The IUS is also know as the ?hormonal coil?. It’s a small soft plastic device that’s place inserted the womb. You don’t have to remember to take it everyday unlike the pill, and it lasts from 3 to 5 years depending on the type of device. It can be removed at any stage, and your fertility levels return to normal.?The IUS can be used by women of all ages regardless of whether you have had a child or not. The IUS has the added benefit that it can make your periods lighter, and it’s often used as a treatment for heavy periods. You can also safely breastfeed with the IUS.
There’s the Intrauterine device (or IUD). This is also referred to as the ?non-hormonal coil?. Similar to the IUS, it’s placed inside the womb. It’s great for people who want to completely avoid hormones, and it can last up to 10 years. Its important to be aware that your periods may become heavier and more prolonged with this device.
The Injection contains the hormone progesterone. It needs to be given every three months. There are just a few caveats to be aware of with the injection. Firstly there is a delay in return to normal fertility after stopping your last injection; it can take up to a year for fertility to return to normal.?I always warn my patients not to take the injection for longer than two years, as it can affect bone density and increase your risk of osteoporosis after this time.?There is a tendency for women to gain weight while on the injection.
Lastly, there’s a device called an implant or ?the rod? as it’s sometimes called. This is a soft, plastic rod containing the hormone progesterone. It’s inserted under the skin of the upper arm. It’s effective for up to 3 years once it has been fitted. One of the main things I warn patients about with the implant is that approximately one-third of patients bleed most days of the month. These people are usually very unhappy with this side effect, and this is the most common reason for women requesting it to be removed.
Over a third want more information about contraceptive options 70% of women haven’t heard of Long Acting Reversible Contraception
7. Which form of contraception is best in terms of limited side effects? Is barrier contraception still the most reliable?
It really depends on the person. That’s why a women’s contraceptive choice is really individual. A contraceptive that causes side effects for one, may not cause any problems for another.?Generally the higher the dose of the hormone in a contraceptive, the more likely it is to cause side effects. Although this isn’t always the case.
Non-hormonal methods like condoms and the copper coil don’t contain any hormone. Because of this, women who want to avoid all hormones or who feel they cannot tolerate hormones might prefer these.?The IUS releases a tiny amount of hormone and acts locally in the womb, so hormonal side effects are unusual.
8. Do you find that women don’t become informed on such topics until it comes to family planning?
Yes, completely. It’s often not until women are having children and spacing their family that they talk among their friends about what contraception they’re using. In Ireland, women are now having their children in their 30’s. I find my female patients in their 30’s are more aware of LARC compared to my patients in their 20’s.
9. Is there any risk with remaining on a contraceptive pill for too long? Should we be giving our bodies a break?
There’s no need to give your body a break from contraception as long as you’re healthy, a non-smoker and your weight is within normal limits. For example, we advise women who smoke and who are over 35 to come off the pill for safety reasons.
There’s one other thing to watch for and that is: you shouldn’t take the injection for more than 2 years at a time because after this time it starts to reduce bone density which may increase the risk of osteoporosis.
10. What’s the most common misconception about birth control options?
There are many, but two big ones that spring to mind are: that you need to take a break from the pill and that the pill gives protection from sexually transmitted infections.?Oh! and that LARC is only for women who have had children.
11. What advice do you have for someone who’s having a bad time on their contraceptive pill, is it a case of changing to another pill or considering a different option altogether?
It could be either. Again it completely depends on the women and her lifestyle. If a patient of mine leads a hectic life and worries about missing a pill and absolutely doesn’t want a pregnancy, then I’d probably guide her towards a LARC ?fit and forget? option.?If the woman is keen to stay on the pill but is having mood swings or an acne breakout, then it may be worth trying a lower dose pill if that’s what she would prefer.
12. How do you know what will agree with your body?
You don’t really know until you try it. Having said that there are some people who should never go on a combined pill. Examples of this would be someone with a family history of a clotting disorder, someone with liver disease or any cancer.?Usually about three months after starting a contraceptive, we’ve a good idea whether it suits or not.
Building on more than 50?years of experience, Bayer HealthCare is committed to improving?all aspects of women’s health. The Truth Report aims to expose existing myths and misconceptions around sex and contraception to inform new thinking, reshape women’s perspective and move the conversation forward, encouraging women and HCPs to engage in a dialogue and share the truth around sex and contraception.
For more information, please see www.mycontraception.ie